June 2021
This month, we spoke with Aleece Fosnight, a sexual health practitioner providing all-inclusive urologic care. Fosnight introduces the concept of the biopsychosocial lens, and how it can inform and improve trans health care.
Aleece Fosnight, MSPAS, PA-C, CSC, CSE has been a physician assistant for the past 10 years and has been a sexual health counselor and educator for almost six years. Aleece opened up her own private practice in June 2020, the Fosnight Center for Sexual Health, in Asheville, NC. She is a provider of comprehensive sexual and reproductive health, basic urologic care, and gynecological care for Western North Carolina and the Southeast U.S.
Fosnight provides all-inclusive urologic care to all generations. Her interests include pelvic floor dysfunction, biofeedback, urinary incontinence, urodynamics, pelvic organ prolapse, pelvic pain, low libido, interstitial cystitis, menopause, female sexual health, low testosterone, and erectile dysfunction. She is also a nationally certified sexual health counselor and educator, providing sexual health education, information, and personalized counseling to patients of all ages.
SHWI: How did you become interested in focusing your practice on trans sexual health? Also what is the prevalence of this population and at what rate is it growing?

In 2012, there was a trans health conference – which has always been an area of interest of mine – in the city near me. During the presentation, one of the physicians commented on the fact that there were too few specialists in the area to take care of trans folx with urinary concerns. Being in urology, I was puzzled why there were no urologists that were willing to see these individuals. So, I went up afterward and introduced myself and said I am here to help, how can we collaborate? We set up a lunch, discussed how we could work together, and our practice started to get referrals. Knowing that this population has unfortunately many barriers to healthcare, I started researching more on trans health and what I could do. And the rest is history! I have been taking care of trans individuals with everything from hormone care all the way to performing orchiectomies as a first-step gender affirming surgery.
In most population surveys, transgender individuals are underrepresented. Estimates of the number of transgender adults significantly increased over the past decade, with a current best estimate of 390 per 100,000 adults. That is about 1 in every 250 adults, or almost 1 million Americans.(1)
SHWI: Why do you believe that a multidisciplinary approach is important for transgender sexual treatment and what kinds do you focus on?
A collaborative approach is really best for all people. In our practice at Fosnight Center for Sexual Health patients get the knowledge base of the medical brain, the physical therapy brain, and the mental health brain; a truly biopsychosocial triad. For trans care, this is especially helpful as they undergo the medical treatment, the physical changes, and the mental challenges and triumphs that come along with transitioning. Our physical therapists address the musculoskeletal changes, tissue morphology, nerve involvement, and post-operative care as needed for healing and function.
As the PA (physician assistant) and sexuality counselor, I am able to provide medical treatments and interventions, diagnostic procedures, simple gender affirming surgeries, and support while they explore their body and partnered relationships. Our mental health providers are able to support our trans individuals with family dynamics, work changes, and navigating the world as an out transgender person. When you provide a collaborative team approach, research shows us that there are better patient outcomes, more efficient treatment strategies, and overall patient satisfaction. And, when you incorporate the patient into a multidisciplinary team, they feel heard, valued, validated, and a part of the decision-making process.(2)
SHWI: Studies show that the trans population struggles more significantly with depression, anxiety, and even higher suicide rates. Why do you think this is true and what kinds of therapy should all practitioners be aware of for this population?
Many of the reasons are likely related to a lack of safety in their environment, their relationships, in their own bodies, and even within the healthcare atmosphere. When they aren't able to get the care they need to transition, it can – for some – feel like they are locked in a body that is not their own. There are constant barriers to them receiving inclusive care: insurance limitations/ being uninsured, lack of competent providers, lack of a support system, financial difficulties, lack of access, and so many more.
So, what should we do as health practitioners? Be aware of the signs/symptoms and have resources for the patient, even if that means having people as referrals to send them to when in need. Providers should seek out training related to trans care or at minimum ensure they know the guidelines for treatment in their scope of practice. For all healthcare providers, crisis management and training in trauma-informed care should be mandatory, as well as required continuing education.
SHWI: Because many healthcare providers are unfamiliar with the transgender transition process, it has been recommended that candidates for surgery take hormones for at least a year. What other best practices should healthcare providers be aware of?
We follow many trans health guidelines at our practice, including: WPATH (World Professional Association for Transgender Health) (3); UCSF (University of California, San Francisco)(4); and Fenway Health (5). As a healthcare provider, it is my responsibility to at least have an overview of all healthcare diagnosis and treatment. As a PA (physician assistant) I am trained in general medicine, which allows me an overall working knowledge of the majority of healthcare concerns. Even though I work in urology and gynecology, if a patient comes to me with depressive symptoms, I should be able to recognize those symptoms and address, acknowledge, and refer out when necessary. Just like trans health, all providers should have some working knowledge or know who to refer to. Here are some of my best practice recommendations:
- Ask all patients about their pronouns
- Ask all patients what name they would like to use
- Ask all patients, “Is there anything else that I can help you with today?”
- Ensure that all restrooms are “All Genders”
- Educate your staff and other colleagues
- General understanding of drug interactions with trans hormone regimens
- Ask who is their support system and do they feel safe where they work and live
- Ask about sexual practices (some trans individuals are sex workers – ask about PrEP and PEP, as well as discuss safer sex practices)
- Ask about tobacco, alcohol, and recreational drug use
- Make follow-up visits more often – assessing for side effects, support system, and mental health is essential and needs to occur more frequently
- Look at your paperwork – is it inclusive? If not, change it
- Consensual exams – always asking permission throughout the entire physical exam, especially during pelvic exams.
- Use gender-neutral language when addressing genital concerns.
- For example, use canal instead of vagina, erectile tissue for clitoris or penis, external folds or external skin for labia or scrotum, internal/external gonads for ovaries or testes
- Intimate partner violence is higher in trans individuals – ask about this at every visit
- Ask about mental health including depression, anxiety, suicidal ideation, isolation, fear, grief, and loss
SHWI: You teach on topics such as looking at sexual health cases through a biopsychosocial lens. Can you explain more about this education and why it’s important for healthcare providers to know?
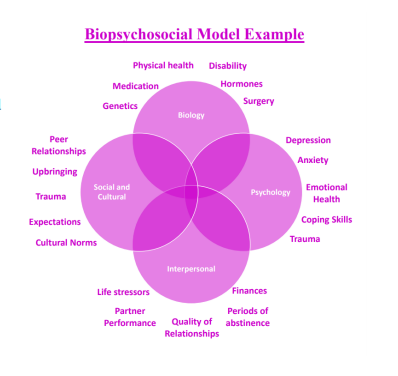
Working through case studies is a way for us to explain our rationale for treatment, our approach to care, and hopefully guide others in their own practice. We hope to aid others by sharing our experience and explaining how we work as a team to gain the best outcomes for our patients. By showing our team approach, hopefully we empower others to seek out providers in their area with whom they can collaborate and co-treat with as well. When you assess a concern through a biopsychosocial lens, you see the whole picture and the influences in that person’s life that are greatly impacting the ability to reach their goal. Here is an example (6):
SHWI: What other important research in the trans medicine field would you like to share with us, either work that you or others have done?
Tracy Sher and Heather Edwards are part of Pelvic Guru, where they push boundaries in presenting education and material relevant to pelvic health PTs and other pelvic health professionals. They have provided several trans-inclusive healthcare models as well as pelvic health in trans individuals both pre- and post-surgical interventions.
At the Fosnight Center for Sexual Health, we continue to evaluate our current process and ensure that we are providing optimal care to all our patients, especially our trans and non-binary folx, as well as access to services. We are in the process of developing sensitivity training for other medical offices and clinics, and biopsychosocial guidelines for trans or gender non-conforming individuals for other multidisciplinary centers to be able to access and model. You can find more information for both patients and healthcare providers on our website.
Sources
1. Meerwijk EL, Sevelius JM. Transgender Population Size in the United States: a MetaRegression of Population-Based Probability Samples. Am J Public Health. 2017;107(2):e1-e8.
2. Rosell, L., Alexandersson, N., Hagberg, O. et al. Benefits, barriers and opinions on multidisciplinary team meetings: a survey in Swedish cancer care. BMC Health Serv Res 18, 249 (2018).
3. Standards of Care for the Health of Transsexual, Transgender, and Gender Nonconforming People, The World Professional Association for Transgender Health
4. Guidelines for the Primary and Gender-Affirming Care of Transgender and Gender Nonbinary People, University of California, San Francisco
5. Transgender Health, Fenway Health
6. Pahwa P.K., Foley S.M. (2017) Biopsychosocial Evaluation of Sexual Dysfunctions. In: IsHak W. (eds) The Textbook of Clinical Sexual Medicine. Springer, Cham.

